Psoriasis ungueal
Enfermedad ungueal psoriásica
Revisado por pares por Dr Colin Tidy, MRCGPÚltima actualización por Dr Doug McKechnie, MRCGPLast updated 17 Abr 2023
Cumple con las directrices editoriales
- DescargarDescargar
- Compartir
- Language
- Discusión
- Versión en audio
En esta serie:La psoriasisPsoriasis en gotasArtritis psoriásica
Psoriasis is a persistent (chronic) skin condition which tends to flare up from time to time. About half of the people who have psoriasis also have changes affecting their nails. Psoriatic nail disease is very variable in appearance and severity.
Psoriasis affecting the nails can be mild and not need any treatment. More severe nail psoriasis is often difficult to treat but modern treatments can be effective.
En este artículo:
Video picks for Problemas de uñas
Continúa leyendo abajo
What is nail psoriasis?
Psoriatic nail disease is a type of psoriasis. It is not caused by infection and you cannot pass it on to anyone else.
Psoriasis is a common skin condition that usually causes patches (plaques) of red, scaly skin but sometimes affects the nails and cuticles. There is also a form of arthritis that is linked to psoriasis, called psoriatic arthritis. Psoriatic nail disease is particularly common if you have psoriatic arthritis. You can read more about these conditions in the separate leaflets called La psoriasis y Artritis Psoriásica.
What causes nail psoriasis?
Volver al contenidoNail psoriasis is caused by the same processes as psoriasis elsewhere. Skin cells grow abnormally rapidly, causing a layer of immature, poorly-functioning skin cells to emerge on the outermost layer of the skin. The immune system is involved in this process, as it seems to attack healthy skin cells by mistake, and trigger skin cells to divide and grow too quickly.
The symptoms and signs of nail psoriasis depend on which part of the nail is affected by psoriasis. For example:
If the nail matrix - the part which produces new nails - is affected, small areas of abnormal cells develop in patches on the nail. As the nail grows, those patches deepen and cause pitting of the nail plate (the hard part of the nail).
If an area of psoriasis grows in the nail bed (the area beneath the nail plate), it can push the nail plate up, detaching the nail plate from the nail bed (onycholysis).
Continúa leyendo abajo
What does nail psoriasis look like?
Volver al contenidoUña psoriásica
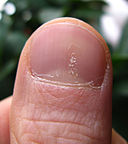
© Seenms, CC BY-SA 3.0, vía Wikimedia Commons
Nail psoriasis can affect fingernails and toenails. There are different types of nail changes that can occur. Signs of nail psoriasis include:
Pitting of the nails
Small pits appear on the surface of the nail. There may be one pit or many pits on the surface of a single nail.
Onycholysis
The nail separates from the skin underneath the nail. At first this looks like a white or yellow patch at the tip of the nail. This patch gradually gets bigger and reaches the base of the nail. The gap between the nail and the skin underneath the nail can become infected and change colour.
Subungual hyperkeratosis
A chalk-like material builds up under the nail. The nail becomes raised and often tender.
Oil drop or salmon patch - a see-through yellow-red patch appears in the nail bed that looks like there is a drop of oil under the nail.
Color
The colour of the nail may change, such as turning to yellow-brown.
¿Qué más podría ser?
Volver al contenidoInfecciones of the nail can occur at the same time as psoriatic nail disease and can sometimes look like nail psoriasis. Infecciones fúngicas de las uñas also cause thickening of the nails. It is important to get the correct treatment as some treatments for fungal nail diseases (eg, terbinafina) can aggravate nail psoriasis.
Onycholysis is the loosening or separation of the nail from the skin underneath it. Treatment depends on the cause. Apart from nail psoriasis it has many other causes - for example:
Trauma to the nail bed - for example, by repeated tapping of the fingernails on a keyboard or by pressure from shoes in long-distance runners and walkers.
Allergy to nail glue (acrylate).
Infections, such as fungal infections, bacterial infections, or the cold sore virus (herpes simplex).
Many medicines - for example, some forms of quimioterapia for cancer, and tetraciclina and fluoroquinolone antibiotics.
Other diseases, such as diabetes o enfermedad tiroidea.
In most of these situations the onycholysis is not permanent and the nail will grow out normally once the cause has been removed or treated.
Continúa leyendo abajo
How common is nail psoriasis?
Volver al contenidoAbout 1 in 50 people have psoriasis at some time in their lives. It can first develop at any age but it most often starts between the ages of 15 and 30 years. Nail changes occur in about half of all people with psoriasis, so about 1 in a 100 people get nail psoriasis.
About 4 in every 5 people with psoriatic arthritis have psoriatic nail disease. Consulte el folleto separado llamado Artritis Psoriásica para más detalles.
Only a few people have psoriatic nail disease without having psoriasis affecting either their skin or their joints.
How is psoriatic nail disease diagnosed?
Volver al contenidoThe diagnosis of psoriatic nail disease is usually made by the appearance of the affected nails. Sometimes scrapings from under the nail, and nail clippings, are sent to the laboratory to be tested for fungal infection of the nail, which can sometimes look like psoriatic nail disease.
Occasionally, a sample of nail (a biopsy) is needed to confirm the diagnosis.
How to help nail psoriasis
Volver al contenidoKeep your fingernails and toenails as short as possible - long or loose nails are more likely to catch and can cause more damage to the skin underneath the nail.
Keep your nails dry.
Protect your nails and wear gloves when doing any manual work.
Avoid a manicure of the base of the nail. This may cause an infection.
Avoid false nails as they may damage the cuticle and make it difficult to apply treatments to the nail.
Nail varnish can be used to cover up pitting. Nail varnish remover containing acetone should not be used, as it can cause damage to the nail.
If you have painful toenail psoriasis then you should see a person who is qualified to diagnose and treat foot disorders (a podiatrist).
Nota: if you have psoriatic nail disease and develop pain or swelling in one or more of your joints (including your fingers and toes) or if you develop pain in your heel (tendinopatía de Aquiles) then you should see your doctor as soon as possible. You may be developing artritis psoriásica. It is important that you are seen by a doctor specialising in joint diseases (a rheumatologist) early. It has been shown that the sooner this condition is treated, the less likely you are to suffer permanent damage to your joints.
How to treat nail psoriasis
Volver al contenidoMild nail disease which isn't causing discomfort does not need any treatment. If the nail disease is severe and causing problems then your doctor may refer you to see a skin specialist for advice and treatment. Unfortunately treatment of psoriatic nail disease is difficult and not always successful.
Treatments for nail psoriasis include:
Treatments applied to the nail, which include esteroides, salicylic acid, calcipotriol o tazarotene. Local treatments applied to the nail are often not very effective in treating nail psoriasis but are worth trying. If the nail is lifting off (onycholysis) then strong steroid scalp application can be trickled under the nail.
Antifungal treatment - this may be required for fungal nail infection if this is also present.
A steroid injected into the nail - this may be effective for some types of nail psoriasis but it is painful.
Light therapy (phototherapy) - psoralen plus ultraviolet light A (PUVA) treatment is effective for some types of nail psoriasis but not for pitting of the nail.
Removing an affected nail - this can be done by applying a special type of ointment and then covering the nail for seven days. Otherwise the nail can be surgically removed using local anestésico.
Patience is important. Once the nail has formed, nothing can be done to change it other than trimming it. The treatments are all aimed at treating the nail bed and the skin around the edge of the nail. Nails grow extremely slowly and it may take as long as a year for a damaged fingernail to grow out completely, or even two years for a damaged big toenail.
If nail psoriasis is severe and not helped by the treatments listed above then a powerful medicine which can suppress inflammation is sometimes used. For example, metotrexato, ciclosporin, acitretina, infliximab, etanercepto, efalizumab, ustekinumab or adalimumab. There is some risk of serious side-effects with these medicines, so they are only used on the advice of a specialist and usually when there is psoriasis also affecting the skin.
What is the outlook (prognosis) for nail psoriasis?
Volver al contenidoNail psoriasis can be difficult to treat and there is no cure. It doesn't usually grow out without treatment, so can continue to cause problems. The appearance of the affected nails can also sometimes cause distress.
The treatment of severe psoriatic nail disease is now improving with modern medicines.
Psoriatic nail disease can also be mild, not needing any treatment, and able to be hidden with nail varnish.
Patient picks for Problemas de uñas

Salud de la piel, uñas y cabello
Infección de uñas por hongos
La infección por hongos en las uñas (tinea unguium) es común, especialmente en las uñas de los pies en personas mayores. La infección causa uñas engrosadas y antiestéticas que a veces se vuelven dolorosas. La medicación a menudo funciona bien para eliminar la infección, pero es posible que necesite tomarla durante varios meses o más.
por la Dra. Philippa Vincent, MRCGP

Salud de la piel, uñas y cabello
Paroniquia
Paronychia is a common infection of the skin around the nails of the fingers or toes. It may be acute or chronic. Treatment is not always needed but usually involves antibiotic medicines for bacterial infections. Occasionally antifungal medicines for infection caused by a yeast (candida) are used. Occasionally steroid creams may be used for the skin around the nail. Rarely a small operation is needed to drain the pus that may have collected.
por la Dra. Philippa Vincent, MRCGP
Lecturas adicionales y referencias
- Psoriasis: La evaluación y el manejo de la psoriasis; Guía Clínica NICE (octubre 2012 - última actualización septiembre 2017)
- Psoriasis ungueal; DermNet NZ
- Ventura A, Mazzeo M, Gaziano R, et al; New insight into the pathogenesis of nail psoriasis and overview of treatment strategies. Drug Des Devel Ther. 2017 Aug 30;11:2527-2535. doi: 10.2147/DDDT.S136986. eCollection 2017.
- Psoriasis - psoriasis ungueal; Sociedad de Dermatología de Atención Primaria. Última actualización mayo de 2022.
- Pasch MC; Nail Psoriasis: A Review of Treatment Options. Drugs. 2016 Apr;76(6):675-705. doi: 10.1007/s40265-016-0564-5.
- La psoriasis; NICE CKS, septiembre 2022 (acceso solo en el Reino Unido)
Continúa leyendo abajo
Historial del artículo
La información en esta página está escrita y revisada por pares por clínicos calificados.
Próxima revisión: 15 Abr 2028
17 Abr 2023 | Última versión
20 Nov 2012 | Publicado originalmente
Escrito por:
Dr Colin Tidy, MRCGP

Pregunta, comparte, conecta.
Navega por discusiones, haz preguntas y comparte experiencias en cientos de temas de salud.

¿Te sientes mal?
Evalúa tus síntomas en línea de forma gratuita
Suscríbete al boletín de Patient
Tu dosis semanal de consejos de salud claros y confiables, escritos para ayudarte a sentirte informado, seguro y en control.
By subscribing you accept our Política de Privacidad. Puedes darte de baja en cualquier momento. Nunca vendemos tus datos.