Enfermedad de Bowen
Revisado por pares por Dr Hayley Willacy, FRCGP Última actualización por Dr Doug McKechnie, MRCGPLast updated 9 Ene 2024
Cumple con las directrices editoriales
- DescargarDescargar
- Compartir
- Language
- Discusión
- Versión en audio
En esta serie:Tipos de cáncer de pielPrevención del cáncer de pielCáncer de piel tipo melanomaCáncer de piel no melanoma
La enfermedad de Bowen es una forma muy temprana de cáncer de piel. Causa uno o más parches pequeños de piel roja y escamosa. Ocurre cuando las células cancerosas de la piel crecen en la capa externa de la piel, pero no se extienden más profundamente en la piel ni a otras partes del cuerpo. Debido a que estas células cancerosas permanecen en la capa externa de la piel, no causan problemas graves por sí mismas. Sin embargo, con el tiempo, existe la posibilidad de que estas células se desarrollen en un tipo diferente de cáncer de piel, lo que puede causar problemas. Por lo tanto, la enfermedad de Bowen generalmente se trata para evitar que esto suceda. Se necesita un seguimiento cercano después del tratamiento para verificar cualquier regreso (recurrencia) de la enfermedad de Bowen.
En este artículo:
Video picks for Erupciones cutáneas
Continúa leyendo abajo
What is Bowen's disease?
Bowen's disease occurs when there is a growth of cancer cells in the outer layer of the skin (epidermis). These cancer cells stay within the outer layer of the skin. Unlike most forms of cancer, these cells can't spread elsewhere. So, Bowen's disease itself is not serious. However, there is a small risk that, over time, it can develop into a more advanced form of skin cancer, which does cause problems.
Is Bowen's disease skin cancer?
Bowen's disease is a very early form of skin cancer. In Bowen's disease, skin cancer cells grow in the outer layer of the skin, but do not grow (or 'invade') deeper into the skin.
Bowen's disease is also called "cutaneous squamous cell carcinoma in situ". Cutaneous squamous cells are cells that make up the outer part of the skin. (Different types of squamous cells are also found in other organs). Carcinoma means cancer, and 'in situ' means 'in place'. In Bowen's disease, squamous cell cancer cells are found in the outer layer of the skin (the epidermis), which is where they originally started growing, but don't spread elsewhere.
Sometimes, Bowen's disease is called a 'pre-cancer', because a key feature of cancers is that they invade other tissues and spread elsewhere in the body - which Bowen's disease doesn't do. Bowen's disease can, however, develop into a - a 'true' form of skin cancer. This happens to about 3 out of every 100 people with Bowen's disease, over time.
What are the symptoms of Bowen's disease?
Volver al contenidoBowen's disease is typically a red-looking patch of skin that has an irregular outline.
The patch can also be:
Crusty or scaly.
Cracked or ulcerated.
Flat or raised.
Sangrado.
Patches can slowly enlarge. Patches of Bowen's disease may be a few millimetres in diameter but, in some cases, can grow to several centimetres.
Sometimes, in its early stages, Bowen's disease can be mistaken for other skin problems such as tiña, psoriasis o eczema discoide.
The picture shows a typical patch of Bowen's disease.
Bowen's disease skin patch

© Crop by Mikael Häggström, from original by Klaus D. Peter, Gummersbach, Germany, CC BY 3.0 DE, via Wikimedia Commons
Bowen's disease more commonly appears on areas of the skin that have been exposed to the sun. In the UK in about three quarters of cases, it occurs on the leg, below the knee. It may also appear on the neck or face, which is more common in Australia and the USA.
It may also be found:
Under or around nails.
On the palms of hands.
On the soles of feet.
Around the back passage (anus).
In the genital area.
Bowen's disease-type skin patches that occur on the genital areas may be given some different names. For example, Bowen's disease that occurs on the penis is called 'erythroplasia of Queyrat'.
Most people just have one patch of Bowen's disease but 1 to 2 people in 10 can have more than one patch at the same time
Continúa leyendo abajo
Cuándo ver a un médico
Volver al contenidoSee a doctor if you think you might have Bowen's disease. If it is, they can offer you treatment to get rid of it.
If a patch of Bowen's disease starts to become ulcerated, bleeds, or if a small bump appears, this could possibly be a sign that it has started to change into a skin cancer. See your doctor as soon as possible if this happens.
Bowen's disease affecting the genitals or anus may be more likely to develop into a skin cancer than Bowen's disease in other places.
What causes Bowen's disease?
Volver al contenidoA patch of Bowen's disease can appear for no apparent reason and can affect anyone. However, there are a number of different things that are thought to increase your risk of developing Bowen's disease. These include:
Long-term sun exposure. Also, use of sunbeds.
Previous radiotherapy treatment - for example, for cancer.
Inmunosupresión. If you have a weak immune system for any reason, this can increase your risk of Bowen's disease. For example, if you have AIDS, if you are undergoing treatment for cancer, have had an organ transplant, or have had medicines to suppress your immune system.
Infection with the vacunas contra el virus del papiloma humano (VPH). It is thought that HPV may be involved in the development of both genital Bowen's disease and Bowen's disease affecting other parts of the skin. HPV type 16 is most commonly associated.
A previous injury to the skin. If you have had an injury to your skin that has caused persistent (chronic) skin damage or scarring, this may increase your risk of developing Bowen's disease in that area.
Inflammatory skin conditions. Rarely, people with chronic skin inflammation problems such as eczema can develop Bowen's disease.
Continúa leyendo abajo
How common is Bowen's disease?
Volver al contenidoAround 15 per 100,000 people in the UK are thought to develop Bowen's disease each year.
It tends to be more common in:
Women more than men.
People aged in their 60s.
People with white skin.
On parts of the body where the skin has been exposed to the sun.
You may also be more likely to develop Bowen's disease if you have previously had one of a group of skin cancers called non-melanoma skin cancers. These are skin cancers that are not malignant melanoma. They include basal cell carcinoma and squamous cell carcinoma. See the separate leaflet called Non-melanoma Skin Cancer for more details.
You are also more likely to develop a non-melanoma skin cancer if you have had Bowen's disease. This is probably due to excessive sun exposure being a risk factor for both Bowen's disease and non-melanoma skin cancers.
How is Bowen's disease diagnosed?
Volver al contenidoBowen's disease is usually suspected by its typical appearance on the skin. Sometimes, to make a diagnosis, a small sample of skin (a biopsia) may be taken. This is then examined in a laboratory. Bowen's disease will have a typical appearance when examined under a microscope.
What is the treatment for Bowen's disease?
Volver al contenidoTreatment can depend on a number of different things, including the site of the patch of Bowen's disease, its size and thickness and how many Bowen's disease patches you have.
The treatment options include:
Observation ('watch and wait')
This may be an option in some people. For example, this may be advised if you have a slowly growing, thin patch of Bowen's disease on an area of your body where skin healing may be difficult (such as your shin). The skin on your shins is very thin and delicate which means that healing can take longer.
Creams applied to the skin
Certain creams may be used in the treatment of Bowen's disease. These can help to kill and get rid of the abnormal cells in some cases. Such creams include 5-fluorouracil (5-FU), a type of chemotherapy cream.
5-FU cream may need to be applied once or twice a day for around three to four weeks and sometimes for longer. The cream is easy to apply yourself. The problem is that it can be quite an irritant to the skin. Your skin may become red and may actually look worse when you are using the treatment.
Treatment may need to be repeated at a later date if the patch of Bowen's disease comes back. 5-FU treatment may be particularly useful in large patches of Bowen's disease or in areas where skin healing may be poor, such as your shin (as explained above). It may also sometimes be used in people who have a number of different patches of Bowen's disease.
Imiquimod cream is also sometimes used to treat Bowen's disease.
Crioterapia
Cryotherapy may be a treatment option in some cases. It is a type of 'freezing' treatment and usually liquid nitrogen is used. Treatment can sometimes be uncomfortable and ulceration of your skin is a possible side-effect.
Curettage treatment
Curettage means that the patch of Bowen's disease is 'scraped' off your skin. A local anaesthetic is used to numb your skin for curettage to be done. Your skin is left to heal naturally and usually a scab forms after treatment and then drops off. There may be less pain during curettage treatment than with cryotherapy.
Cirugía
In some cases, surgery to remove the patch of Bowen's disease may be suggested. For example, surgery is usually carried out for Bowen's disease around the back passage (anus).
The patch of Bowen's disease is cut out from your skin under local anaesthetic and stitches are used to close up your skin again afterwards. Skin healing may sometimes be difficult, especially when surgery is used to remove patches of Bowen's disease on the leg below the knee.
Terapia fotodinámica
This has been used with some success to treat Bowen's disease. Photodynamic therapy is carried out by applying a special chemical to the patch of Bowen's disease. The chemical is photosensitive, which means it reacts to light.
A special light source is then directed at the affected patch of skin to activate the photosensitive chemical. This then makes it burn and destroy the patch of Bowen's disease.
Sometimes burning and stinging of the area of skin being treated can occur and your skin may become irritated. Rarely, skin colour may be lost or, in some cases, become darker in the treatment area.
Radioterapia
Radiotherapy is treatment with X-rays. It is another treatment option for Bowen's disease but it is less commonly used than other treatments, and usually only used if other treatments haven't worked. Again, radiotherapy may not be suitable to treat Bowen's disease below the knee because of problems with skin healing after treatment.
Tratamiento con láser
This is also sometimes used to treat patches of Bowen's disease.
Can Bowen's disease be prevented?
Volver al contenidoBecause excessive sun exposure is the most important risk factor for developing Bowen's disease, we should all limit our sun exposure in the summer months (or all year when in hot countries nearer the equator) by:
Staying indoors or in the shade as much as possible between 11 am and 3 pm.
Covering up with clothes and a wide-brimmed hat when out in the sunshine.
Applying sunscreen of at least SPF 15 (SPF 30 for children or people with pale skin) which also has high UVA protection.
If you have had Bowen's disease, you should make sure that you check your own skin regularly for any changes.
¿Cuál es el pronóstico?
Volver al contenidoWith most treatments for Bowen's disease, there is probably about a 1 in 10 chance that Bowen's disease will come back (recur) after treatment. Therefore, regular follow-up is needed to look for any signs of recurrence. Further treatment may be needed if this happens.
The outlook for most people with Bowen's disease is very good. The vast majority of people who have Bowen's disease that is recognised and treated will not develop a skin cancer.
Understanding the skin
Volver al contenidoThe skin has two layers - the outer layer (epidermis) and the inner layer (dermis). Beneath the dermis is a layer of fat and then the deeper structures such as muscles and tendons.
Vista en sección transversal del diagrama de la piel
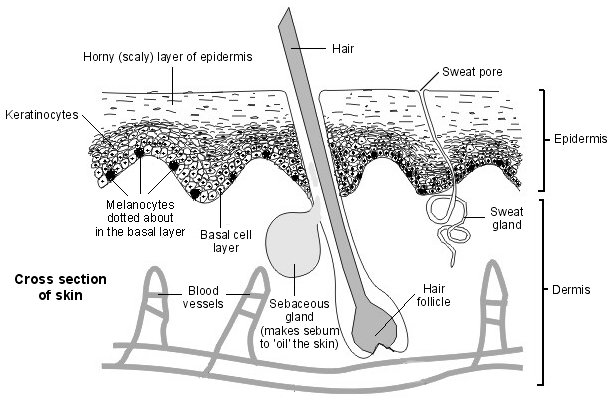
The epidermis has three main types of cell:
Basal cells. These are the bottom layer of cells in the epidermis.
Keratinocytes. These cells are in layers above the basal layer. They make a substance called keratin which is a hard waxy material. Keratinocytes are constantly dividing and a certain number are dying at any given time. The top (horny) layer of the epidermis is made of dead keratinocytes which contain keratin. The top of the skin is constantly being shed and replaced by new dead cells which contain keratin.
Melanocytes. These cells are dotted about at the bottom of the epidermis. They make a pigment called melanin when skin is exposed to sun. The melanin is passed to the nearby skin cells to protect them from the sun's rays. Melanin causes the skin to tan in fair-skinned people. Dark-skinned people have more active melanocytes.
Patient picks for Erupciones cutáneas

Salud de la piel, uñas y cabello
Sarpullido por calor y sudamina
La erupción por calor es uno de los tipos más comunes de erupción cutánea, y también se conoce como miliaria, sudamina o sarpullido por sudor. La erupción por calor ocurre en algunas personas cuando sudan mucho. Puede ser muy pruriginosa. Se debe a un bloqueo de los conductos sudoríparos que hace que el sudor se filtre en las células de la piel. El tratamiento principal es mantenerse fresco tanto como sea posible.
por la Dra. Rosalyn Adleman, MRCGP

Salud de la piel, uñas y cabello
Queratosis actínica
Una queratosis actínica (también conocida como queratosis solar) es la afección cutánea más común causada por el daño solar. Es el resultado de que la piel se dañe por el sol durante muchos años. Las queratosis actínicas suelen ser parches ásperos y escamosos en áreas expuestas al sol, como la cabeza y la cara. Las queratosis actínicas son comunes, especialmente en personas mayores, muchas de las cuales tienen más de una. Por lo general, son inofensivas, pero existe un pequeño riesgo de que eventualmente se conviertan en cáncer de piel y, por lo tanto, se puede aconsejar tratamiento.
por el Dr. Doug McKechnie, MRCGP
Lecturas adicionales y referencias
- Terapia fotodinámica para tumores de piel no melanoma (incluyendo lesiones precancerosas y primarias no metastásicas de la piel); Guía de procedimientos intervencionistas de NICE, febrero de 2006
- Bowen's Disease - non-genital; DermNet NZ
- Bath-Hextall FJ, Matin RN, Wilkinson D, et al; Interventions for cutaneous Bowen's disease. Cochrane Database Syst Rev. 2013 Jun 24;(6):CD007281. doi: 10.1002/14651858.CD007281.pub2.
- Sharma A, Birnie AJ, Bordea C, et al; British Association of Dermatologists guidelines for the management of people with cutaneous squamous cell carcinoma in situ (Bowen disease) 2022. Br J Dermatol. 2023 Feb 10;188(2):186-194. doi: 10.1093/bjd/ljac042.
Continúa leyendo abajo
Historial del artículo
La información en esta página está escrita y revisada por pares por clínicos calificados.
Próxima revisión: 7 de enero de 2029
9 Ene 2024 | Última versión

Pregunta, comparte, conecta.
Navega por discusiones, haz preguntas y comparte experiencias en cientos de temas de salud.

¿Te sientes mal?
Evalúa tus síntomas en línea de forma gratuita
Suscríbete al boletín de Patient
Tu dosis semanal de consejos de salud claros y confiables, escritos para ayudarte a sentirte informado, seguro y en control.
By subscribing you accept our Política de Privacidad. Puedes darte de baja en cualquier momento. Nunca vendemos tus datos.